Quick Takeaway
- Don't quit cold: Stopping abruptly can cause withdrawal symptoms in up to 86% of patients.
- Half-life matters: Drugs like paroxetine need slower tapers than fluoxetine.
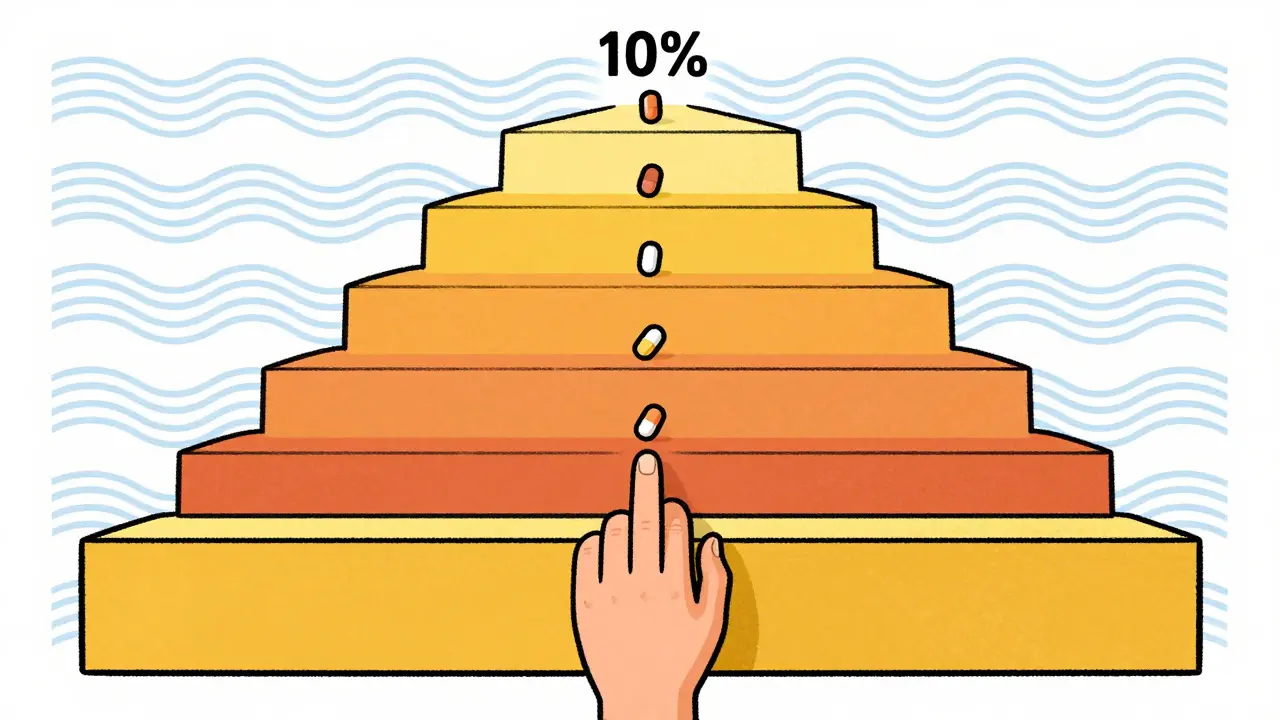
- The 10% Rule: Reducing doses by 10-25% every few weeks is standard practice.
- Last 10% is critical: The final stage of tapering often causes the most severe symptoms.
- Track your progress: Dizziness and 'brain zaps' are common but manageable signs.
Stopping antidepressant medication is rarely a simple act of just putting the last pill down and forgetting about it. Your brain gets used to the chemical presence of these drugs over time. If you suddenly remove them, that balance shifts violently. This isn't just feeling a bit moody; it is a physiological reaction known as Antidepressant Discontinuation Syndrome (ADS). Studies suggest that anywhere between 27% to 86% of people experience some form of withdrawal when they stop too quickly.
So, why do we rush into this? Often because people feel better and assume they are cured, or because side effects became bothersome. But rushing off treatment leads to a high chance of relapse. Research shows that stopping maintenance therapy without a proper plan increases the risk of depression returning within two years to around 60%. You aren't just trying to avoid feeling sick in week one; you are securing long-term stability.
Understanding the Mechanism Behind Withdrawal
To understand why a schedule matters, you have to look at what happens inside your system. Most commonly prescribed antidepressants work by adjusting neurotransmitters like serotonin. When you take them daily, your brain adapts. It changes receptor sensitivity to maintain homeostasis. When you stop taking the drug, the receptors are suddenly overwhelmed or under-stimulated, leading to the symptoms you feel.
This is where the concept of Half-life becomes your best friend or worst enemy. Half-life is simply the time it takes for the concentration of a drug in your blood to reduce by half. Some drugs leave your body very fast. Others linger for days. If a drug leaves your system quickly, your brain feels the absence immediately.
For example, Fluoxetine (Prozac) has a unique property among its peers. It stays in your system for a long time because its active metabolite remains active for several days. This acts as a natural buffer. Because of this, many people can switch off fluoxetine with fewer immediate withdrawal spikes compared to other options. On the other end of the spectrum sits Paroxetine. With a short half-life of roughly 21 hours, it clears out rapidly. This means skipping a single dose or stopping too fast triggers symptoms much faster and more intensely. Meta-analyses show paroxetine causes discontinuation symptoms in 44% of abrupt stoppers versus just 18% for fluoxetine users.
Designing Your Tapering Schedule
There is no one-size-fits-all button to press here. However, clinical guidelines provide a framework that drastically reduces risk. The golden rule cited in resources like the Australian Prescriber and various psychiatric handbooks is to reduce your dose gradually. A common standard recommendation is cutting your current daily dose by 10% to 25% every 1 to 4 weeks.
Why the range? It depends on how your body reacts. If you cut by 25% and feel fine after two weeks, you might proceed. If you get dizzy, nauseous, or start seeing 'electric shocks' in your head (often called brain zaps), you need to pause. Sometimes you even need to step back up to the previous level until symptoms fade before trying again.
| Strategy | Suitability | Risk Level | Typical Duration |
|---|---|---|---|
| Direct Switch | Long half-life drugs only | High | < 1 Week |
| Taper & Switch | Most SSRIs | Medium | 2-6 Weeks |
| Ultra-Slow Taper | Long-term users (5+ years) | Low | 12+ Weeks |
While the table above gives you the options, the "Ultra-Slow" approach is gaining traction for patients who have been on medication for a long time. Research indicates that users on antidepressants for five years or more face higher risks of severe and prolonged withdrawal. Their nervous systems have adapted more deeply to the drug's presence. For these individuals, a slow taper of less than 10% reductions over months is becoming the new standard of care.
Navigating the "Last Mile"
Many people make it through the big cuts but crumble at the finish line. Experts like Dr. James Davies have noted that the final stages of the process are disproportionately difficult. Specifically, the last 10% of the dose reduction is responsible for up to 50% of withdrawal symptoms. Why? Because as your dose gets smaller, percentage drops represent smaller absolute milligram amounts, yet the receptor occupancy changes non-linearly.
This is where tablet formulations become tricky. You cannot split a 20mg tablet down to 20 tiny pieces easily. Precision becomes an issue. That is why switching to liquid formulations or compounded medications can be a game-changer near the end. A study from King's College London found that being able to reduce doses by precise 1mg increments reduced severe withdrawal symptoms by 62% compared to standard tablet splitting.
If you are stuck at the end, ask your doctor about a liquid option. It allows you to titrate the dose down by just a fraction every couple of weeks rather than waiting weeks for a massive 10% drop that might shock the system.
Managing Cross-Tapers and Switches
What if you aren't stopping because you feel done, but because the current drug isn't working well enough? Switching medications requires similar caution. You generally shouldn't just pop off one and start another. There are four main protocols observed in clinical settings:
- Direct Switch: Abruptly stopping Drug A to start Drug B immediately. Only safe if Drug A has a very long half-life.
- Taper & Switch Immediately: Gradually reducing Drug A and starting Drug B on the same day.
- Cross-Tapering: Slowly lowering Drug A while simultaneously increasing Drug B over 1-2 weeks.
- Washout Period: Stopping Drug A completely and waiting before starting Drug B.
You need to pay close attention to the washout period, especially if moving between classes like MAO inhibitors. If you are switching from an MAOI, you usually need a 14-to-21-day washout period to avoid something dangerous called serotonin syndrome. Conversely, switching from venlafaxine to sertraline usually follows a cross-taper method where you lower venlafaxine by ~37.5mg every few days while boosting sertraline by 25mg over the same timeline.

Recognizing the Signs: Withdrawal vs. Relapse
One of the biggest hurdles is telling the difference between withdrawal symptoms and the return of depression. They can look identical. Both involve sleep issues and mood swings. However, there is a timing clue. Withdrawal symptoms usually appear very quickly after a dose drop-within a week or even a few days. Relapse tends to develop more slowly over time.
A major study highlighted by Harvard Medical School tracked hundreds of patients and found that physical symptoms like dizziness, nausea, and sensory disturbances were hallmarks of withdrawal, whereas emotional heaviness persisting without physical triggers suggested relapse. Despite this distinction, 73% of patients experiencing discontinuation symptoms mistakenly think they are relapsing. This fear often sends them back to restarting the full dose immediately, which undoes the progress. Education is vital here. If you feel weird after dropping a dose, try slowing the taper rate rather than quitting entirely.
Frequently Asked Questions
How fast should I taper my antidepressant?
General guidelines suggest reducing your dose by 10% to 25% every 1 to 4 weeks. However, this varies by drug and individual tolerance. Short half-life drugs require slower tapers.
Can I stop antidepressants cold turkey?
No, abrupt cessation is strongly discouraged. It significantly increases the risk of withdrawal symptoms (up to 86%) and relapse (60% recurrence risk). Always consult a doctor for a plan.
Which antidepressant is hardest to stop?
Drugs with short half-lives like Paroxetine and Venlafaxine are notoriously difficult to stop due to rapid clearance from the body. They trigger symptoms faster than longer-lasting drugs like Fluoxetine.
Is there a test to predict withdrawal severity?
Emerging pharmacogenetic testing looks at CYP2D6 and CYP2C19 metabolizer status. Early studies suggest this predicts about 38% of the variance in withdrawal symptom severity.
What helps if I feel worse during the last stage?
If symptoms flare up, hold your current dose until they stabilize. Using liquid formulations to make tiny dose adjustments (micro-tapering) can help navigate the final 10% of reduction safely.
Remember that this journey is personal. While guidelines provide the math, your body provides the answer. Listening to your own signals and keeping open communication with your healthcare provider ensures you reach the finish line without unnecessary suffering.

Christopher Curcio
March 30, 2026 AT 14:22The pharmacokinetics involved here are nontrivial regarding serotonin transporter modulation and receptor downregulation patterns observed in chronic SSRIs administration. Half-life variance dictates the kinetic profile of discontinuation syndrome manifestation across different patient populations. Neurotransmitter homeostasis disruption occurs rapidly when elimination rates exceed compensatory mechanisms significantly. We see significant differences between drugs with active metabolites versus those lacking secondary stability pathways entirely.
Calvin H
April 1, 2026 AT 14:14The idea that a quick fix exists for neurological dependency is genuinely amusing given how complex neurochemistry actually works.
Beccy Smart
April 2, 2026 AT 03:33I totally get what you mean about the complexity though 🧠💊 People just want the magic pill gone and done 😅😌 It is scary seeing the side effects stats up close ⚕️ Hope everyone finds a good schedule 💪
Angel Ahumada
April 2, 2026 AT 23:57one must consider the epistemological weight of prescribed chemical interference upon the autonomous mind and its subsequent attempt at reclaiming sovereign integrity through gradual cessation protocols that ignore social constructs of recovery speed we accept blindly in modernity
Katie Riston
April 4, 2026 AT 03:17We often overlook the profound philosophical implications of altering our baseline chemistry.
The body seeks homeostasis at all costs regardless of external medication.
Removing a substance changes the equilibrium permanently in subtle ways.
It reminds me that our mental state is fluid rather than static.
Many patients ignore the slow dance of receptor resensitization entirely.
This process requires patience beyond mere clinical guidelines.
Nature reclaims balance when artificial support vanishes too quickly.
Withdrawal isn't weakness but a physical recalibration mechanism.
We must respect the nervous system as an adaptive organism constantly evolving.
Rushing the decline creates unnecessary trauma for the biological machinery.
The final percentage drop hits harder because adaptation lags behind dosage reduction.
Liquid formulations offer a precision that pills simply cannot match near the end.
Ignoring these details leads to suffering that could have been avoided easily.
True healing involves listening to the signals sent by the internal physiology.
Understanding the timeline helps manage expectations during the transition period.
Ruth Wambui
April 5, 2026 AT 23:57Big Pharma loves selling you the problem and then the solution while keeping you dependent forever for profit margins instead of health outcomes. They design meds that require cold turkey stops to force relapse and renewal of prescriptions. Trust the system less and trust your own bodily intuition more regarding these dangerous chemicals.
sanatan kaushik
April 6, 2026 AT 09:50You speak nonsense about the doctors who help people survive severe depression episodes without medication assistance. I tell you medicine saves lives daily and ignoring science makes people suffer longer than necessary. Listen to the professionals before you go chasing wild theories about corporate evil plots.
RONALD FOWLER
April 8, 2026 AT 00:07its tough to stop taking something that keeps you stable but pushing through is worth it in the end i believe in your strength always remember you do not have to do this alone
stay strong and take care of yourself
Carolyn Kask
April 9, 2026 AT 19:27Americans need to learn discipline instead of coddling every little withdrawal symptom with endless talk therapy and micro-dosing nonsense. Real men and women finish the treatment plan without whining about brain zaps for months on end. Stop making excuses and commit to the process fully.
Rick Jackson
April 10, 2026 AT 07:23Patient progress varies widely depending on individual biology and duration of usage history.
Debbie Fradin
April 10, 2026 AT 21:07Oh sure because biology fixes itself on a neat timeline like everything else in life. That is dangerously optimistic thinking for someone who hasn't felt the full weight of a crash firsthand. You are ignoring the reality of suffering that happens when the math does not align with human experience.
Vikash Ranjan
April 11, 2026 AT 17:52Why does everyone assume slower is always better when some bodies clear toxins faster than others without issue. Maybe the guidelines are too conservative for healthy individuals who metabolize drugs differently than average study subjects.
William Rhodes
April 12, 2026 AT 08:39Keep fighting through whatever stage you are in right now because victory waits for those who persist despite discomfort. Your mind is stronger than any chemical reaction and you will regain your freedom eventually with proper pacing.